Syncope
Syncope, or blackouts, has many potential underlying causes. The clinical history is crucial in understanding the mechanism of collapse and when advising treatment options. Episodes of syncope may be associated with prior dizzy spells, light-headedness, palpitation or frequent falls and should undergo detailed specialist assessment.
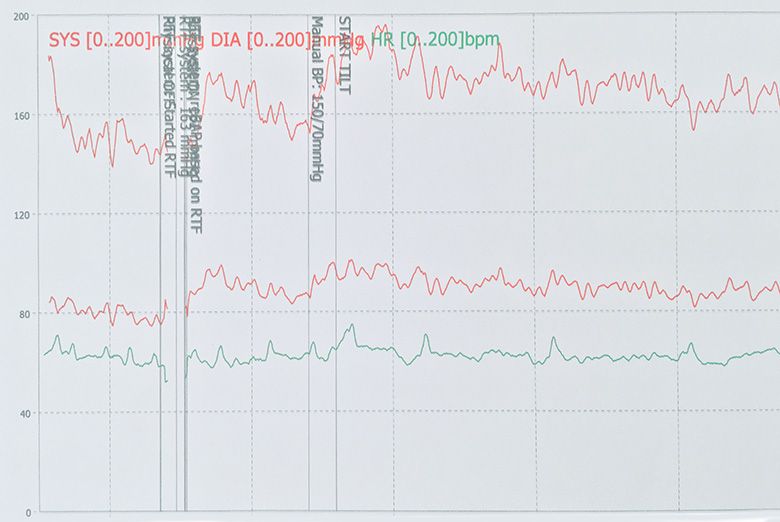
Tilt table test
Investigation of syncope usually entails blood tests, a 12-lead Electrocardiogram (ECG), Echocardiogram, prolonged ECG holter monitoring and certain patients may require a tilt-table test. Insertion of an implantable ECG loop recorder, a day case procedure performed under local anaesthetic, is available for patients suspected to have an underlying arrhythmic cause for syncope.
Management of syncope is dependent on the underlying cause and severity of the condition. Vasovagal syncope, or 'simple' fainting, for example is a common cause and may be triggered by several factors including warm environments, dehydration and emotional stimuli. Postural orthostatic hypotension describes a significant fall in blood pressure on standing and can also cause syncope. These two forms of fainting may be manageable by simple lifestyle modification, patient response to warning symptoms and adjustment to existing prescribed medication. Some patients however may require specific additional medication such as Fludrocortisone or Midodrine to increase blood pressure in order to improve symptoms.
Syncope can also be caused by specific cardiac conditions that require prompt investigation and treatment including arrhythmia, cardiomyopathy or severe heart valve disease. A concerning cause for syncope is bradyarrhythmia (abnormal slow heart rate), such as sinoatrial node disease or complete heart block. In these situations, a permanent pacemaker procedure could be recommended and may be required on an emergency basis.
If syncope is felt to be life threatening, such as hypertrophic cardiomyopathy with ventricular arrhythmia, insertion of an implantable cardioverter-defibrillator may need to considered. An underlying cause of severe valvular disease, such as aortic stenosis, may require urgent consideration of heart valve replacement.


